If you’re not sure that bilateral salpingectomy is the right surgery for you, please read the female sterilization procedures overview page.
On this page, we discuss the bilateral salpingectomy in the context of pre-surgery, during surgery, post-surgery, and recovery. Follow the linked pages to find out more detailed information.
Overview
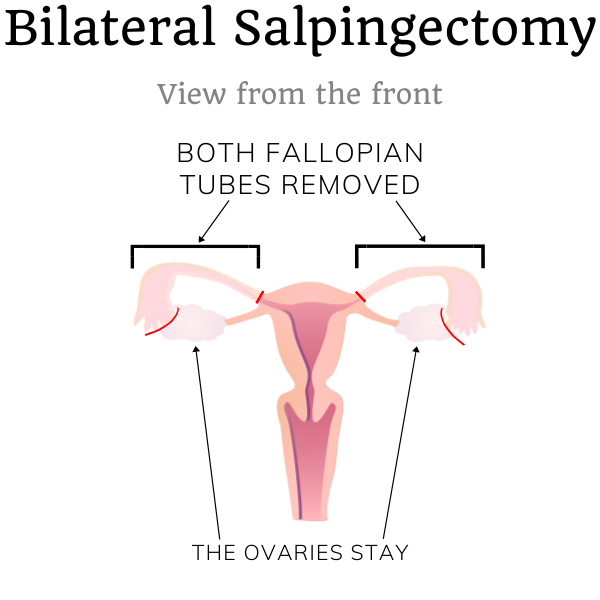
Bilateral salpingectomy is another common method to sterilize women. Besides preventing pregnancy, a bilateral salpingectomy can also reduce the risk of future ovarian cancer development 1.
Bilateral means on both sides of the body. Salpingectomy means the surgical removal of the fallopian tubes. The fallopian tubes are also known as the uterine tubes and the salpinges. Sometimes, people call it a tubectomy instead of a salpingectomy, though they may also conflate bilateral salpingectomy with bilateral tubal ligation. Because a few bilateral tubal ligation methods also remove part of the tube, the difference can get a bit fuzzy.
The fallopian tubes are about 11 to 12 centimeters2 long. Any removal of a piece of tube is a salpingectomy, which is why it’s helpful to look at salpingectomy as a spectrum. Anything less than the whole tube can be called a partial salpingectomy. In this article, we assume you’re undergoing a full bilateral salpingectomy with no fallopian tube left in your body on either side.
Doctors perform this procedure worldwide. Depending on the hospital and your doctor, you can undergo this surgery by laparoscopy or laparotomy. A few factors will change the outcome in hospital time and your surgical scars. The general rule is: if you choose a better hospital with a highly-trained doctor and pay more, you will have less time under anesthesia, less recovery time, and fewer scars. This isn’t a perfect rule, since you can also pay a lot for bad healthcare.
One reason to do a unilateral salpingectomy instead of on both sides of the body is to remove an ectopic pregnancy. It’s a life-saving procedure because ectopic pregnancies are very dangerous to women. Another reason to perform this surgery on one side of the body is to remove an infection of the fallopian tube. This is condition of having a blocked fallopian tube due to an infection is known as hydrosalpinx.
Bilateral salpingectomy is a female sterilization method that is permanent and irreversible. Do not seek out bilateral salpingectomy if you might want to become pregnant later.
Note: if you are pregnant and want this to be your last pregnancy, you can also undergo a bilateral salpingectomy right after giving birth. You must also have discussed this with your doctor prior to giving birth. This will look different from how this page describes bilateral salpingectomy down below.
Undergoing bilateral salpingectomy surgery
Read our guide for what to do for and expect of your female sterilization surgery here.
While you’re unconscious from the general anesthetic, your surgeon will begin your bilateral salpingectomy. This begins with making the incisions for either laparoscopic surgery or laparotomy.
The duration of your surgery depends on a few factors. A laparoscopic bilateral salpingectomy will take about 30-60 minutes while the same procedure via laparotomy takes 45 minutes or more. As a general rule, less time spent under general anesthesia is better for you. This surgical time is slightly more than a bilateral tubal ligation (laparoscopically, 20-30 minutes). But because bilateral salpingectomy provides better protection against both pregnancy and developing ovarian cancer 3, it has become the golden standard for those who wish to be sterile since the 2010s.
If you’ve chosen a laparoscopic bilateral salpingectomy, the surgeon will make a small incision in your navel and a small second (and possibly third) incision below your bikini line. If you’ve chosen a bilateral salpingectomy by laparotomy, your surgeon will make a longer incision below your bikini line. You can find more information about laparoscopic approaches on the page that compares surgical incisions.
Method to remove the fallopian tubes
Once your surgeon has a good view of your womb, your ovaries, and your fallopian tubes, they will begin the sterilization procedure. For a trained gynecological surgeon, removing both entire fallopian tubes is a relatively straightforward surgery. Though one surgeon might have different instruments at their availability than another, the method of fallopian tube removal is the same no matter what. However, it’s still a good idea to ask your doctor about how exactly they perform the procedure since it’s part of your informed consent.
Your surgical team uses various tools to grab your fallopian tubes, hold them down, cut them at both the uterus and the ovary, remove them from your body, stop bleeding, and tidy up. The fallopian tube does not connect to the ovary – instead, it slightly grabs it during ovulation to catch the egg – so the tidying up only happens where the fallopian tube was connected to the uterus and the abdominal tissue called the mesosalpinx. Modern surgical tools both cut and cauterize at the same time, leading to little need for the surgeon to tidy up their work. Instead, they just check everything once they are done before closing up and finishing the surgery.
If you are okay with watching this, here’s a surgery video of a (bilateral) salpingectomy performed in the USA.
Findings during your surgery
Your anatomy is unique. Because your surgeon doesn’t know what they’ll find once they begin the operation, the surgery might turn out a little different than anticipated. For example, if your surgeon finds a cyst on your now-removed fallopian tube or endometriosis on your uterus, they might tell you after the surgery. They could also find other things unrelated to your reproductive health since the surgeon can see other organs, such as your colon, gallbladder, stomach, pancreas, liver, and appendix while performing your bilateral salpingectomy.
If they for example find a cyst, it will likely be sent to pathology for examination. This is a standard procedure. You can inquire after the operation if it went as expected or if your surgeon found some surprises.
The failure rate and pregnancy risk
It’s impossible to become pregnant via sex after a bilateral salpingectomy, so the failure rate stands at 0%. It is considered the most effective form of birth control for people with uteruses.
After your bilateral salpingectomy, you will still ovulate since the ovary is still there. During ovulation, a fertile egg leaves the ovary and goes into your abdominal cavity where it gets reabsorbed by your body. Since there is no fallopian tube anymore to facilitate a meeting between sperm and egg and the access the the uterus is sealed off, you cannot become pregnant anymore.
However, if you have unprotected sex before your bilateral salpingectomy, it’s possible to become pregnant and even carry the pregnancy to term without having fallopian tubes. This, however, does not negate the efficacy of bilateral salpingectomies in preventing pregnancy.
There is no way for your body to ‘regenerate’ an entire fallopian tube (we are not lizards). Hypothetically, if your surgeon did a bad job and didn’t seal off the uterine access, it would be possible for sperm to travel through that hole and find a fertile egg cell floating around the abdomen (peritoneal cavity) aimlessly. However, this would be a non-viable ectopic pregnancy. There is one documented case 4 of a woman falling pregnant after having her last fallopian tube removed. Her early and non-viable pregnancy disappeared by itself. A shoddy salpingectomy surgery is the main theory of how this happened. This one case should not be your deciding factor to pursue or not pursue a bilateral salpingectomy as a form of permanent sterilization.
Risks and contraindications
Since bilateral salpingectomy is abdominal surgery, it comes with a few rare risks and contraindications. All these risks are due to the surgery and anesthesia. The salpingectomy procedure itself doesn’t add any significant risk. Read our page about risks, contraindications, and side effects to learn more.
Conclusion
We hope this page gave you a good overview of the surgical procedure known as bilateral salpingectomy, its method, and its advantages and disadvantages. If you have any questions, don’t hesitate to send us a message.


- Source: https://www.acog.org/clinical/clinical-guidance/committee-opinion/articles/2019/04/opportunistic-salpingectomy-as-a-strategy-for-epithelial-ovarian-cancer-prevention[↩]
- 4.3 to 4.7 inches[↩]
- Source: https://pubmed.ncbi.nlm.nih.gov/28232128/[↩]
- Source: https://www.fertstert.org/article/S0015-0282(04)02993-0/fulltext[↩]